Human blood types have deep evolutionary roots, Science News:
The A, B and O blood types in people evolved at least 20 million years ago in a common ancestor of humans and other primates
O for the German “ohne,” meaning “without” (without the A or B antigen)
Not quite. See below.
Depending on blood type, people are more or less susceptible to particular pathogens. Type O people, for example, are more susceptible to cholera and plague, while people with type A are more susceptible to smallpox.
BLOOD GROUPS [PDF], Stedman’s, which describes itself as:
Welcome to medicine’s most authoritative word reference site
STEDMAN’S® is the authoritative, comprehensive, and trusted brand that the medical community has relied upon for accurate medical information for the past 100 years.
ABO blood group
Cells of type O do not simply lack antigenic substance; most have an antigen called H that is chemically similar to antigens A and B and is probably the precursor antigen that is modified under the influence of genes A1, A2, and B into their corresponding antigens.
The designation “Bombay” phenotype was assigned to those whose cells lack A, B, and H antigen and whose serum contains anti-A, anti-B, and anti-H; they are also referred to as having the “Oh” phenotype. In addition, weak variants of antigen A have been described with phenotypes designated A3, A4, A5, Ax, and Az; more rarely, weak variants of B have been found. The ABO types are of prime importance with respect to blood transfusion, and maternal-fetal incompatibility is a frequent cause of fetal death and erythroblastosis fetalis.
As sober and factual as Stedman’s is, it makes no mention of ABO distribution/frequency differences. It does however mention other racial differences.
Dombrock blood group
This group includes antigens Doa and Dob and is found slightly more often in white patients.
Duffy blood group
Blood from whites is agglutinated by one or both antigens; most blacks, however, and some Yemeni Jews have negative test reactions to both antigens.
Duffy antibodies occasionally cause transfusion reactions or erythroblastosis fetalis.
Gerbich blood group
Incidence of the three high-incidence antigens is found in all populations, except in Melanesians.
Anti-Ge2 and anti-Ge3 are noted to elicit acute reactions on transfusion but have not been identified in hemolytic disease of newborns.
Indian blood group
This is the most recently discovered blood group. It is composed of two antithetical antigens, Ina, which is of somewhat low incidence, and Inb, which is of high incidence (96% of whites, and 96% of Indians).
Anti-Inb has been linked with hemolytic transfusion reactions. Anti-Ina has not been so linked, however. Neither has been linked to hemolytic disease of the newborn.
Sutter blood group
It occurs in about 20% of American blacks but is rare in other ethnic groups. Sutter antibodies have been implicated in transfusion reactions and in hemolytic disease of the newborn
An example of a mixture of smart and stupid when it comes to blood and race. Donors’ Races to Be Sought To Identify Rare Blood Types, 1990:
To ease a chronic shortage of rare blood types, the New York Blood Center will for the first time begin asking donors to volunteer information about their racial and ethnic backgrounds.
The program is to begin on Monday, and scientists at the center say they hope it will enable them to better provide rare blood types, or blood found in one in 10,000 people. The center is especially concerned about groups under-represented by donors, like black and Hispanic groups.
The center does not have the time or the resources to test each of the 2,200 pints it collects daily for every possible type of rare blood, said Dr. Joan Pehta, an associate in immunohematology at the center. If the center knew the races and ethnic backgrounds of donors, she said, then when a call came in for a specific rare type, the center could conduct the manual tests most likely to yield that type.
”For example, the U negative blood type occurs only in black people,” said Dr. W. Laurence Marsh, senior vice president of the center. ”No white person has ever been found to be U negative. It is a blood type just like any other, but it doesn’t occur very much, and if you need U negative for any person, then you have got to have black donors. And so the problem for us is to identify black donors. It makes no sense to screen 100,000 whites for U negative when no U negative white person has ever been found.”
Conversely, only whites have the blood types Vel negative and Lan negative, Dr. Marsh said.
Memories of Segregation
Knowing the ethnic background of a blood donor can also help the blood center.
Center officials concede that because of historical racist segregation of blood, there may be objections to the new program, especially if people do not fully understand it.
But they emphasize that donors do not have to disclose such information for their blood to be accepted. Center officials say that blood banks try to make determinations of race, but usually not through straightforward requests. Some blood centers decide the race of a donor based on appearance, which is at best imprecise.
those who have the greatest difficulty getting the blood they need in an emergency are members of racial or ethnic minorities that do not give blood often.
Andrea Smith, manager of public relations for the blood center, said the blood bank has no data on how much blood is given by people in different ethnic and racial groups because it has never sought that information. The American Red Cross, however, studied donors in the United States in 1986 and found that 95 percent of them were white and 4 percent were black.
In written and oral explanations, the center’s staff will emphasize that while there is no such thing as ”black blood,” ”white blood” or ”American Indian blood,” knowing ethnic and racial backgrounds will help the center quickly provide the right types of blood to those who need them.
At Harlem Hospital, Dr. Helen Richards, director of the blood bank there, and Dr. Leslie Holness, who handles emergency cases, agreed that the center’s approach might be helpful to black and Hispanic patients who have trouble getting the blood they need.
Racial and Ethnic Distribution of ABO Blood Types, BloodBook.com:
There are racial and ethnic differences in Blood type and composition.
As the chart below reveals, the frequency and purity of the four main ABO Blood groups varies in populations throughout the world. Great variation occurs in different groups within a given country; even a small country, as one ethnic group mixes, or not, with another. Blood type purity depends on migration, disease, interrelational-reproductive opportunity, traditions and customs, geography and the initial Blood type assigned.
Publishing the ethnic differences in Blood type and the racial differences in Blood type is not, in the present-day world, considered to be politically correct. We compile and maintain this database through and thanks to, often times, reliable, confidential sources. Every Blood gathering entity in the world must gather this information to stay in business, but almost every one of them is afraid to publish the racial and ethnic differences in Blood type, given the emotionally charged political climate.
For example, early European races are characterized by a very low type B frequency, and a relatively high type A frequency while the Asiatic races are characterized by a high frequency of types A and B.
Everyone carries substances on their red Blood cells, called antigens. In addition to the well known ABO classified groupings, and Rh factor, there are over 260 “minor” antigens that have been identified. These antigens may appear in varying combinations. The presence or absence of these specific “minor” antigens single out that particular Blood type as being “rare.” All Blood types are inherited and therefore certain rare Blood combinations are more common in specific ethnic and racial groups.
There is precise and up-to-date data available. These racial and ethnic Blood typing and population migration statistics are important in modern medicine for many reasons. The overriding problem in obtaining and publishing this information in the United States, and to a slightly lesser extent in Western Europe, is political correctness. It is not nice to talk about the ways that I may be different from you!
Chart shows ABO frequencies for a large variety of racial strains.
Rare Blood Types, BloodBook.com:
All Blood belongs to a major group: A, B, AB, or O. However, there are more than two hundred minor Blood groups that can complicate Blood transfusions.
It is also very important to know the race or ethnic background of a Blood donor or candidate for a Blood transfusion. The Blood center physician, or Blood bank technician must always be alert for special Blood types. Your Blood type is inherited just like the color of your eyes and hair. Many Blood types, therefore, are found only in specific racial and ethnic groups. For example listed here is a very few of the most common Blood types in the most often seen rare ethnic categories:
-
African American Blacks – U- and Duffy-
-
American Indians and Alaskan Native peoples – RzRz
-
Pacific Island peoples and Asians – Jk ( a- b- )
-
Hispanics – Di ( b- )
-
Russian Jews – Dr ( a- )
-
Whites – Kp ( b- ) and Vel
Blood and Diversity, American Red Cross, provides the same table as above. Also:
Importance of Type O
Different ethnic and racial groups also have different frequency of the main blood types in their populations. For example, approximately 45 percent of Caucasians are Type O, but 51 percent of African Americans and 57 percent of Hispanics are Type O. Type O is routinely in short supply and in high demand by hospitals – both because it is the most common blood type and because Type O-negative blood, in particular, is the universal type needed for emergency transfusions. Minority and diverse populations, therefore, play a critical role in meeting the constant need for blood.
This is exactly the opposite of the truth. They don’t donate. They play a critical role in the constant need for blood, not in meeting that need.
Duffy antigen system, Wikipedia:
Duffy antigen/chemokine receptor (DARC) also known as Fy glycoprotein (FY) or CD234 (Cluster of Differentiation 234) is a protein that in humans is encoded by the DARC gene.
Polymorphisms in this gene are the basis of the Duffy blood group system.
Population genetics
Differences in the racial distribution of the Duffy antigens were discovered in 1954, when it was found that the overwhelming majority of blacks had the erythrocyte phenotype Fy(a-b-): 68% in African Americans and 88-100% in African blacks (including more than 90% of West African blacks).[39] This phenotype is exceedingly rare in whites. Because the Duffy antigen is uncommon in those of Black African descent, the presence of this antigen has been used to detect genetic admixture.
“Population genetics” is a euphemism for race.
In the Yemenite Jews the frequency of the Fy allele is 0.5879[46] The frequency of this allelle varies from 0.1083 to 0.2191 among Jews from the Middle East, North Africa and Southern Europe. The incidence of Fya among Ashkenazi Jews is 0.44 and among the non-Ashkenazi Jews it is 0.33. The incidence of Fyb is higher in both groups with frequencies of 0.53 and 0.64 respectively.[47]
These Duffy-related genetic differences express themselves in other significant ways.
Clinical significance
Asthma
Asthma is more common and tends to be more severe in those of African descent.
Benign ethnic neutropenia
A significant proportion (25–50%) of otherwise healthy African Americans are known to have a persistently lower white blood cell count than the normal range defined for individuals of European ancestry—a condition known as benign ethnic neutropenia. This condition is also found in Arab Jordanians, Black Bedouin, Falashah Jews, Yemenite Jews and West Indians.
HIV infection
A connection has been found between HIV susceptibility and the expression of the Duffy antigen.
Prostate cancer
Experimental work has suggested that DARC expression inhibits prostate tumor growth. Men of black African descent are at greater risk of prostate cancer than are men of either Causcasian or Asian descendant (60% greater incidence and double the mortality compared to Caucasians).
Transfusion medicine
A Duffy negative blood recipient may have a transfusion reaction if the donor is Duffy positive.[40] Since most Duffy-negative people are of African descent, blood donations from people of black African origin are important to transfusion banks.
The Diego blood group, NCBI Bookshelf:
The Diego blood group was discovered in 1955
In 1967, a second Diego antigen, Dib, was discovered. It wasn’t until 1995 that other Diego antigens began to be discovered.
The longer scientists look at blood, the more differences are discovered.
Number of antigens – 21: Dia, Dib, and Wra are among the most significant
Molecular basis
The SLC4A1 gene encodes the Diego antigens.
Located on chromosome 17 (17q21-22), the SLC4A1 gene contains 20 exons that span more than 18 kbp of DNA. The alleles Dib and Dia result from a SNP (2561C→T), and the corresponding Dib and Dia antigens differ by a single amino acid (P854L).
Frequency of Diego antigens
Dia is found mainly in populations of Mongolian descent. It is found in 36% of South American Indians, 12% of Japanese, and 12% of Chinese, whereas it is rare in Caucasians and Blacks (0.01%). Dib is found universally in most populations (1).
Common phenotypes
The most common Diego phenotype is Di(a-b+), which is found in over 99.9% Caucasians and Blacks, and over 90% of Asians. The Di(a+b+) is found in 10% of Asians. Whereas the Dia antigen is universally expressed in most populations, the prevalence of the Dia antigen differs among races, making the Diego blood group of great interest to anthropologists (3).
In the USA, the Dia antigen has not been found in Caucasian or Black blood donors (4). The Dia antigen is more commonly found in Oriental people of Mongolian descent, being more common in the Japanese (12%) and the Chinese (5%). In South American Indians, up to 54% of the population carries the Dia antigen (1).
Interestingly, the Dia antigen is less rare in the Polish population (0.47%) (5) compared to most Caucasian populations (0.01%). This may reflect the gene admixture that resulted from the invasion of Poland by Tatars (Mongolian heritage) many centuries ago (6).
Revista Brasileira de Hematologia e Hemoterapia – The history of the Diego blood group outlines a progression in the understanding of its distribution and significance:
-
as a “Private Factor”, first identified in a woman named Diego
-
as an “Indian Factor”, found in high concentration among various Amerindian tribes
-
as a “Mongolian Factor”, lower concentrations in broader Mongoloid populations
In 1956, in a paper published in the Nature Journal (5), Layrisse and Arends stated: “Since the Indians of the American continent are considered to be anthropological related to the Mongolian people of the old world, we decided to investigate the incidence of the Diego Factor in other available representative Asians living in Venezuela”.
By 1959:
Many papers showing the distribution of the Dia antigen considered that it was essentially a Mongolian characteristic, absent in Whites , Blacks, Australian aborigines and other populations (10-39).
Here is another example, not discussed in the podcast, of the nonsense generated by anti-“racist” ideology. The American Journal of Color Arousal: “Race” and Blood Types, Superstition and Science, by Francis L. Holland, a pro-black political activist/blogger. From the sidebar:
Human Genome Project Disproves Concept of “Race”
In other words, the Human Genome Project has proven that, as a matter of scientific fact, that which we call “race” does not exist as a matter of biology, and so all references to “race” are references to a fallacy.
This is the same technique used in “The Races of Mankind” – making bald assertions while fraudulently invoking science for support. Holland, however, goes beyond “race isn’t significant” and claims “race does not exist”.
Blood differences are expressions of underlying genetic differences – racial differences, fine and coarse. The racial nature of these differences, and others, are generally euphemized, minimized, or denied. This is a direct consequence of anti-“racist” ideology and politcal pressure, not lack of evidence. When racial differences are acknowledged, as for example by the Red Cross or New York Times, the discussion is specifically justified by the perceived benefit for non-Whites. Anti-“racism” is properly understood as anti-Whitism.
Would you rather have a blood transfusion from someone who shares your skin color or from someone who shares your blood type? It is my belief that transfusing blood from one person to another based on skin color would be an extraordinarily dangerous practice.
Blood science is one of the better examples that race runs deeper than skin color. Based on a scientific understanding of blood compatibility the optimal source for donors follows a racial progression of increasingly-looser genetic proximity: yourself, your family, your tribe, your ethny, your (continental) race. Every source beyond yourself, even a sibling, requires additional screening for antigen compatibility.
The anti-“racist” notion that blood type is only ABO is analogous to their notion that race is only skin color. In these cases, and others, they are obviously trying to minimize differences.
Holland cites the Red Cross table cited in Part 1:
The blood table below, broken out by “race,” shows that blood types do not obey superstitious sociological and cultural notions of “race”.
As blurry as the Red Cross tries to make it, the coarsest racial differences are still visible. Anti-“racism” is worse than any superstition that springs from the mere absence of evidence. Anti-“racism” is a fantasy maintained by rejecting all evidence to the contrary.
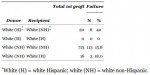
If a white person with type O+ blood needs a battle-field transfusion and medics don’t know the blood types of another white person available and an Hispanic person available, the best bet (53% O+) would be to give the white person a transfusion from a Hispanic person–NOT another white person.
This is the kind of nonsense anti-“racist” obfuscation creates.
If the goal is to improve the chances of finding O+ then you’d want to be more racially specific than “Hispanic”. The “best bet” (100% O+) would be unmixed Amerindians. To maximize the quality and likelyhood of finding a match, even in the general case, it makes more sense to take into account race – biological differences and their varied distributions – than it does to pretend those differences don’t matter.
The podcast will be broadcast and available for download on Tuesday at 9PM ET.
Podcast: Play in new window | Download